PCOS (Polycystic Ovary Syndrome)
I know there are a few of you out there who have it, and it’s something can alter quite a few things with regards to how fast you can see results and how your body is feeling internally.
So grab a drink and sit down for 5-10 minutes and have a read while i share some advice on what you can be doing.
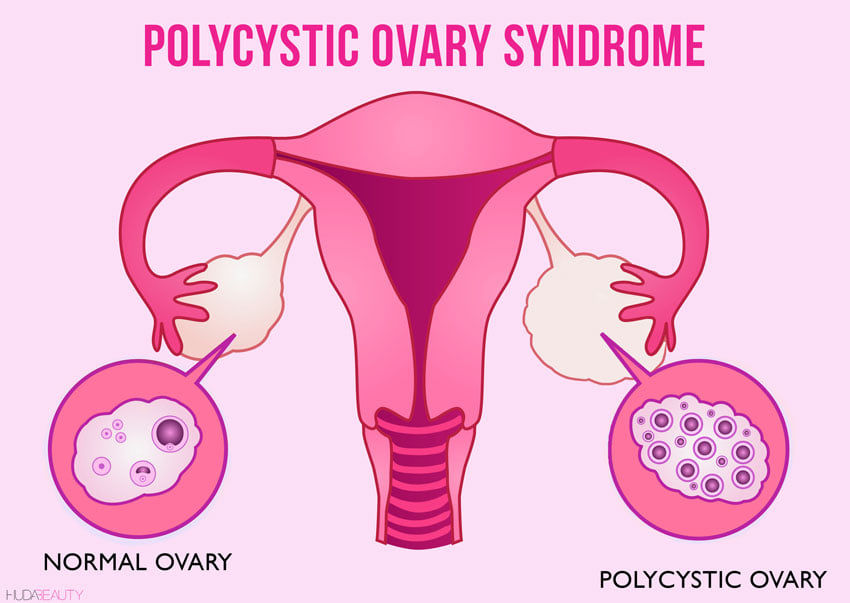
What is it?
Imbalance of reproductive hormones: Excess androgens
How is PCOS diagnosed?
- Multiple small follicles/cysts on the ovaries (seen on an ultrasound)
- Ovarian cysts alone do not = PCOS
- Clinical evidence of elevated androgen levels (hyperandrogenism), identified via:
- Blood test
- Symptoms such as excess facial or body hair growth, hair loss, acne
- Anovulation (lack of, or irregular periods)
What causes PCOS?
Cause unclear
Women with PCOS are 50% more likely to have a mother, aunt or sister with PCOS
Genetics and family history are thought to be associated
Suggested factors:
- Insulin resistance
- Hyperandrogenism from puberty
- Obesity
**We should also be aware, that just because someone has cysts on their ovaries, it doesn’t necessarily mean they have PCOS. Having ovarian cysts is actually quite common and often aren’t harmful (of course these are all points for a patient to discuss with their doctor)
What are some symptoms?
- Irregular or absent menstrual periods (>35 or <21 day cycles)
- Infertility or reduced fertility
- Hirsutism (excessive hair growth related to increased androgens)
- Alopecia
- Acne
- Darkening and thickening of the skin
- Obesity and difficulty losing weight
- Increased risk of miscarriage
Conditions associated with PCOS
Increased risk of:
- Gestational diabetes & type 2 diabetes
- Eating disorders
- Non-alcoholic fatty liver disease
- Mood disorders
- Sleep apnoea
- Cardiovascular disease
- Metabolic syndrome
- Hypothyroidism & autoimmunity
- Endometrial cancer
How to manage it
What we can control
Lifestyle intervention: diet, exercise, behaviour modification
What we can’t control
Cosmetic: laser, waxing, electrolysis
Pharmacological: oral contraceptives, anti-androgens, insulin sensitisers, ovulation induction
Surgical: laparoscopic surgery, bariatric surgery
Dietary management
The nutritional management for someone with PCOS is very individual and will need to be tailored to the persons symptoms, blood work, lifestyle and body.
Impact of weight loss on PCOS
Studies have show a weight loss of even just 5% can help:
- Restore regular menses
- Improve response to ovulation-inducing fertility medications
Overall, in women with PCOS and excess weight, lifestyle interventions which reduced weight by as little as 5% of total body weight have been shown to have healthy metabolic, reproductive and psychological benefits however, dieting has been shown to have negative psychological effects
Up to 70% of Australian women with PCOS are overweight or obese and as we know obesity is associated with a greater degree of insulin resistance, hyper-insulinemia, lipid abnormalities, hyper-androgensim, hirsutism and menstrual irregularities.
Higher prevalence of abdominal body fat distribution, even those of a normal body weight
Dieting has been shown to have negative psychological effects… so again keep in mind that you can shift the goal post to focus on healthy lifestyle and behavioural changes rather than focusing on a weight loss goal.
You may have heard to remove gluten, dairy or soy from your diet? But do you?
Gluten
There’s no evidence of any benefit or harm in women with PCOS consuming gluten, usually sees some improvements because a gluten-free diet often does not replace all gluten-containing grains for gluten-free alternatives, therefore, lowering the carbohydrate intake overall.
Dairy
Milk contains naturally occurring hormones and given PCOS is a hormonal condition, many are concerned about the implications. Evidence is currently inconclusive. A 2013 study of 400 Iranian women of which 40 had PCOS and showed that dairy consumption had no significant effect on PCOS symptoms (Rajaeieh, Marasi, Shahshahan, Hassanbeigi, & Safavi, 2014). There is some evidence to suggest that dairy can exacerbate acne so in this case you could potentially reduce intake to see if there are any improvements rather than cutting it out completely, however keep in mind calcium alternatives would also need to be prioritised.
Soy
Soy can be quite controversial as people seem to worry about the isoflavones which have a similar structure to estrogen and it seems to be one of the most feared foods especially in women’s health. Soy has been found to be beneficial for heart health, helping to improve insulin resistance and there is even some evidence showing a link to improved IVF outcomes (Gaskins & Chavarro, 2018)
So what foods should you be eating/minimising?
Carbohydrates & fibre
Lower carbohydrate might be beneficial for some
- Opt for low GI where possible
- Pair high GI with fat and protein
- Ensure adequate fibre intake
- Diet rich in legumes, pulses, beans
- Aim for 25-30g
Mediterranean style diet
AKA ‘anti-inflammatory style diet’
Dietary approaches high in monounsaturated fats, omega 3’s, fibre and antioxidants appear to assist with managing PCOS symptoms
Mediterranean style diet features:
- High in vegetables, fruits, legumes, wholegrains, fish, poultry and healthy fats such as extra virgin olive oil, avocado, nuts and salmon
- Moderate amounts of red meat, eggs and fermented dairy (yoghurt & cheeses)
- Strongly linked with reduced symptoms of anxiety and depression
What other things should you be including in your weekly meal plan?
Vitamin D
Vit D. has grown in popularity in PCOS treatment
There is some research to suggest supplementation is beneficial for women with PCOS to improve fertility and insulin resistance however again, it will depend on the individual and if its effective for them since there is no formal consensus
Cinnamon
Support menstrual regularity, improve blood sugar regulation, improve cholesterol
Dose: 1-2g/day
Zinc
Reduce androgen related hair growth/loss, may assist with insulin resistance
Supplement dose: 50mg/day
Omega 3’s
Reduces inflammation and improves metabolic markers like cholesterol and blood pressure, may also reduce testosterone and improve regularity of menstrual cycle, only need supplementation if inadequate from diet
Supplement dose: 1000-3000mg
Take a holistic view, rather than just focusing on diet or training alone. What other factors come in to play?
SLEEP
Sleep apnoea is common in women with PCOS
Lack of sleep can:
- Worsen insulin sensitivity
- Increase diabetes risk
- Increase blood pressure
- Associated with weight gain
- Plan strategies with client to improve sleep quality
- Refer on to receive specialist intervention
STRESS
- Increases blood glucose levels
- May lead to emotional eating and weight gain
- May affect fertility
- Recommendations
- Strategies to manage/reduce stress
- Referral to psychologist where appropriate
EXERCISE
- Auto-regulation with training during menstruation
- Exercise will assist with managing blood sugar
- Standard general population exercise guidelines
- 150 min/week of moderate intensity physical activity or 75 min/week of vigorous intensities or an equivalent combination of both
- ‘Muscle strengthening activities’ on 2 non-consecutive days/week
- Setting SMART goals
Hope that helps ladies, and let me know if you enjoyed this article, or if there are any other topics you would love to see me cover 
